In 1997, a large outbreak of hepatitis A was associated with consumption of raw oysters in New South Wales. 
Recent outbreaks have been associated with contaminated shellfish, lettuce, strawberries, river water and blueberries. Since 2010, there has been an average of approximately 20 notified cases per year in Victoria.Ĭommon-source outbreaks, due to food contaminated by an HAV–infected food handler or food (shellfish, raw products) contaminated before entering the food chain, are rare. Sporadic cases occur in childcare centres with children in nappies, travellers to countries where the disease is endemic, people who inject drugs, and men who have sex with men.Īlthough a vaccination program for Indigenous children commenced in Queensland in 1999, Indigenous children remain at greater risk than non-Indigenous children, particularly for hospitalisation with hepatitis A. In industrialised countries, disease transmission is frequently among household and sexual contacts of an acute case. In about half of all Victorian cases, no source is identified. In some South-East Asian countries, more than 90 per cent of the general population can have serological evidence of prior infection with hepatitis A, compared with industrialised countries, with a rate of 33 per cent. When environmental sanitation is poor, infection is common and occurs at a young age. The incidence of disease is related to hygiene and sanitation conditions. Public health significance and occurrence of hepatitis A The incubation period is 15–50 days, with an average of 28–30 days. Rarely, people may have a relapse of acute hepatitis, with a second peak in aminotransferase elevation, or a cholestatic form of hepatitis A with prolonged pruritus. The pattern of liver function tests may be nonspecific in later illness. In the acute stage of the illness, blood biochemistry shows elevated transaminase levels, indicating hepatocellular damage. IgG anti-HAV antibodies alone are evidence of past infection or immunisation. These antibodies are present for 2–4 months after infection and, rarely, can persist for more than 1 year.įalse positive IgM results can also occur, especially in older people, so testing for anti-HAV IgM should ideally be done only when hepatitis A is clinically suspected.Ī fourfold or greater increase in specific antibodies in paired sera detected by enzyme-linked immunosorbent assay (ELISA) also establishes the diagnosis. IgM anti-HAV antibodies become detectable 5–10 days after exposure. The virus can be detected in the blood and stool of most people during the acute phase of infection.Ī blood test indicating IgM anti-HAV antibodies in acutely ill or recently ill patients establishes the diagnosis. The overall mortality rate from hepatitis A is 0.3–1.8 per cent in people aged over 50 years. Rarely, fulminating hepatitis may occur, especially when hepatitis A infection complicates pre-existing liver disease. Symptoms usually last less than 2 months, although 15 per cent of symptomatic people have prolonged or relapsed disease for up to 1 year. 
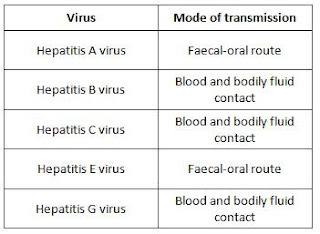
The disease can vary from a mild illness lasting 1–2 weeks to a severely disabling disease lasting several months. Illness due to hepatitis A typically causes fever, fatigue, malaise, anorexia, loss of appetite, nausea, vomiting, abdominal pain, clay-coloured bowel movements, joint pain, and jaundice in more than 70 per cent of patients.ĭark urine usually precedes the development of jaundice, and mild pruritus (itching) may occur. If illness does occur, it is typically not accompanied by jaundice (yellowing of skin or eyes). In children less than 6 years of age, 70 per cent of infections are asymptomatic. Hepatitis A causes acute viral hepatitis and does not lead to chronic hepatitis. Hepatitis means inflammation of the liver. Identification of hepatitis A Clinical features Hepatitis A virus (HAV), a hepatovirus from the Picornaviridae family, is the causative agent, primarily through the faecal–oral route. Exclusion for hepatitis AĮxclude from childcare, school or work (for food handlers, and healthcare workers with direct patient contact) for 1 week after the onset of illness or jaundice and until they are well. This is a Victorian statutory requirement. Pathology services must follow up with written notification within 5 days. Hepatitis A is an ‘urgent’ notifiable condition and must be notified by medical practitioners and pathology services immediately by telephone upon initial diagnosis (presumptive or confirmed).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
